Shocker, if people think they are treated unfairly, it might be bad for their health
What my first published dissertation paper says about healthcare discrimination and heart disease
Disclaimer: The views here do not necessarily express the views of my employer or sponsors.
The point of this essay is to provide an accessible summary of one of my papers. This is the first summary in what I hope to be a series I do for my first author and senior author papers going forward. While a lot of my budding following here are academics, I also hope to reach audiences outside of my of my academic bubble.
Many people talk about communicating research in a way that makes it more accessible. I think this matters. Something that I think matters even more is that research tends to have a life of its own once it goes into the world. Following up my first author and senior author papers with a complementary essay here allows me to control my own narrative a bit. It is also a helpful look-back on the trajectory of my work.
One of my dissertation papers was published today in Circulation: Population Health and Outcomes (formerly Circulation: Cardiovascular Quality and Outcomes). This is the journal of the American Heart Association’s Council on Quality of Care and Outcomes Research.
My main study takeaway is that in the overall sample, discrimination was associated with higher risk of heart attack or stroke. This association persisted when we accounted for an array of sociodemographic factors (namely wealth, marital status, insurance status, education), and health status (namely chronic health conditions and a history of these events). This finding is an interesting signal showing that how people feel in these spaces can serve as a marker for risk.
Relevant disclosure: I serve as a volunteer on the Early Career Committee of the Council on Quality of Care and Outcomes Research (QCOR).
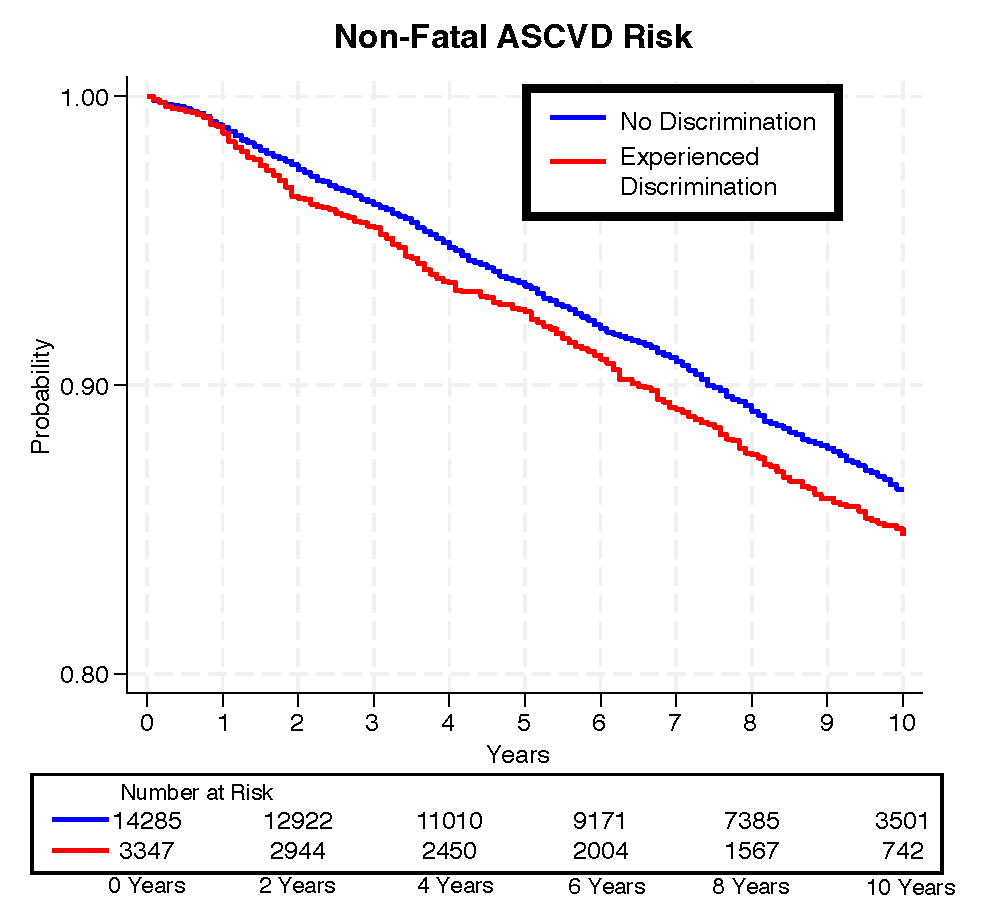
A media headline for this study would be something scary like “RACISM IN HEALTHCARE LINKED TO HIGHER HEART ATTACKS AND STROKES” which is a scary assertion and a misrepresentation of the work. Even though it is a misrepresentation, it is not an unfair assumption to someone who skims the paper. Below is the first figure from this paper. The red line shows those who reported discrimination in healthcare and the blue line shows those who did not report it. This figure shows that those who report discrimination in healthcare are more likely to have a heart attack or stroke over time.
The scale of the risk in between groups is not huge. There are two different ways this could be reported.
1. A hazard ratio tells you how much a single factor increases someone’s risk of having an event. In my study, Table 2 shows the hazard ratio is 1.44 for discrimination in healthcare for all adults. A hazard ratio of 1 means no difference, and anything above 1 means higher risk. So a hazard ratio of 1.44 for discrimination means people who reported discrimination were 44% more likely to have a heart attack or stroke. That assertion without context is scary, but it also is a bit misleading because something like elevated blood pressure (hypertension) is considerably more harmful. We have many tools at our disposal to mitigate those more harmful risk factors (e.g. cheap drugs, lifestyle interventions like exercise, clear dietary guidance) that are much more consequential. Also examining increased risks of events that are (ideally) rare might not amount to health outcomes being noticeably different. The harmful consequences of high blood pressure is a finding repeated across so many studies and has been so consistent in research that clinical guidelines now incorporate it as a major healthcare factor that needs to be addressed. Discrimination in healthcare is nowhere near that level.
2. In the supplemental file of the paper, you can find the adjusted event rates. Over the 10 years of follow-up, you can see that those who did not report discrimination had a 9.97% stroke or heart attack rate, versus a 12.09% stroke or heart attack rate for those who did report discrimination.
For discrimination in healthcare to gain broader recognition as a risk factor for health, findings like the ones in my paper need to show up consistently through repeated studies in different contexts with the same results, be built from well-defined measures of discrimination, and hopefully point toward actionable targets and interventions.
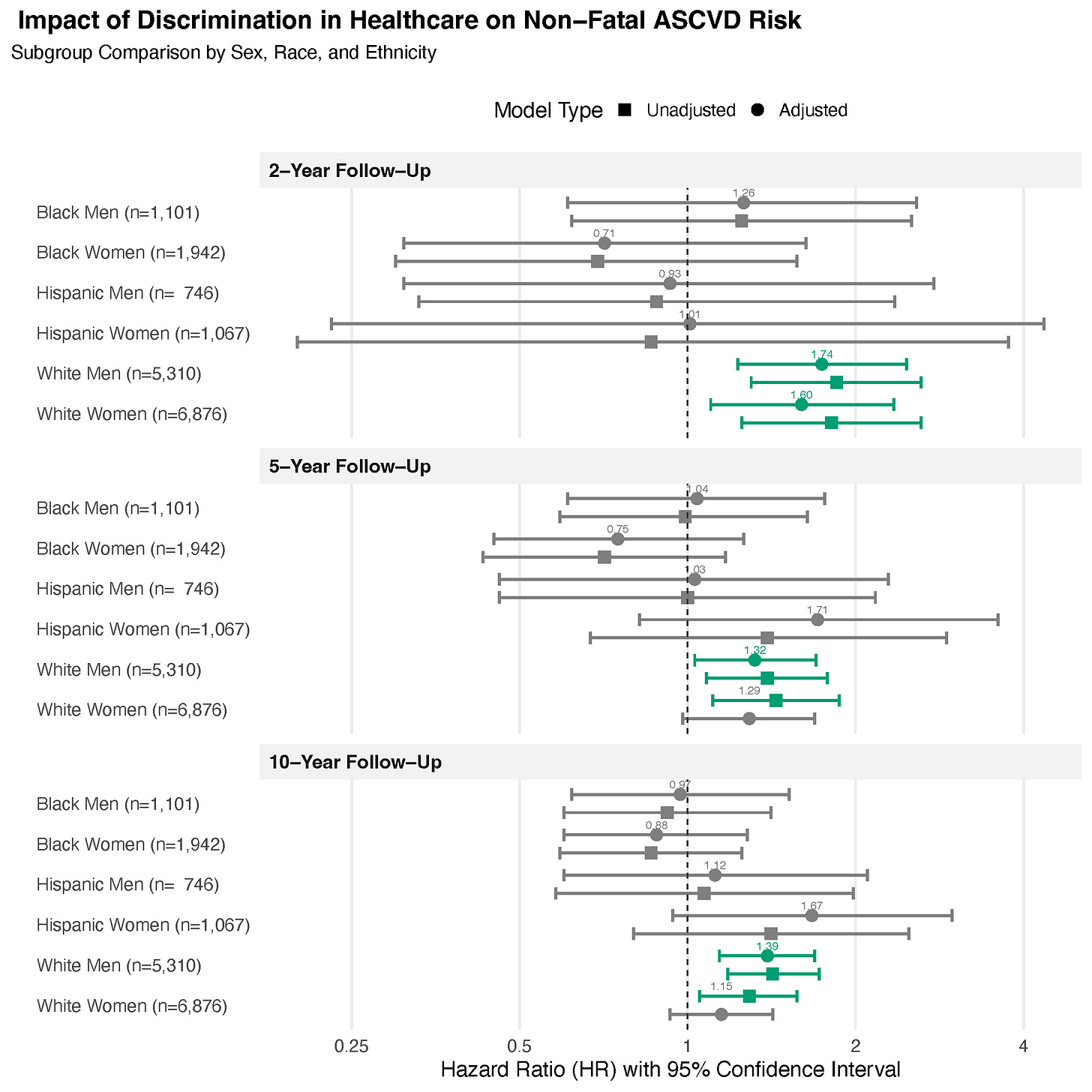
The juiciest (and perhaps most perplexing) finding is illustrated in Figure 2 below.
The way you read this chart is: if the point and confidence interval bars sit to the right of the 1 line, discrimination is a risk factor for that group. If they fall to the left of the 1 line, discrimination appears “protective”. If the group’s confidence interval cross the 1 line, it is not a statistically significant finding.
Through 2, 5, and 10 years of follow-up discrimination was a statistically significant risk factor only for White men, both before and after adjustment for the factors we considered. For White women it was a statistically significant risk factor through 2 years of follow-up but not through 5 or 10-years. Again thinking of how my work could be taken out of context this figure could lead to another scary headline of “RACISM IS ONLY HARMFUL FOR WHITE MEN” which would certainly get clicks but is again a misrepresentation of the study.
My research focuses on discrimination in healthcare, and one of the most visible forms of discrimination comes from recent discourse on racism in healthcare. This is also what people often assume I care about most when they see me, a Black man, or hear about my family’s negative experiences. Racism is a phenomenon which can be more elusive (e.g. someone is denied for a bank loan which they are qualified for, but the determining factor was they were Black). Discrimination in my view is a more overt action (e.g. someone is told that they cannot eat in a restaurant because of some type of attribute). Both can be consequential, we can measure both, but the recording of both and attribution of harm is contested. That assumption might make someone’s eyes glaze over if they are opposed to reckoning with the past and present racial issues in America. It galvanizes a group of people who want to attribute racism as the primary driver of all health disparities. Both viewpoints can lead to blind spots in other forms of mistreatment. My initial hypothesis was that healthcare discrimination reported by self-identified underrepresented racial and ethnic minority adults would be associated with increased risk of stroke or heart attack.
For my analysis, I used two complementary approaches for considering other factors that could contribute to how I interpret any connection between discrimination in healthcare and stroke or heart attack: model adjustment and sample weighting. Model adjustment accounts for specific factors we know are important to consider, like age, smoking status, or prior heart events. Weighting addresses the fact that people who report discrimination may differ systematically from those who do not in ways that could bias our results. By reweighting the sample, we create a comparison that more closely resembles what we would see if discrimination were randomly experienced. Using both together strengthens the analysis because if either approach is slightly off, the other can compensate. Our analysis included around 17,000+ people who answered the question on being unequally treated in healthcare settings, which is a large sample for this type of longitudinal study (a study that follows people over a prolonged period).
Why did I not find what I hypothesized? Maybe it is because there are only a few thousand self-identified racial and ethnic minority individuals in my sample. The longitudinal data in the Health and Retirement Study are powerful, but participating in a survey assumes willingness, availability, and ability to participate. Some might say that discrimination not showing a significant association with risk of heart attack or stroke for Black adults or Hispanic adults means that perceived mistreatment for these individuals does not matter. In my view this makes me want to understand what surrounds these individuals even more. In American healthcare we famously are one of the few nations in the global north without universal healthcare, our social safety net is also notoriously poor and shrinking. However, I would also argue that our interpersonal treatment of individuals today is far better than times such as slavery or the Jim Crow era. There is room to grow because of the high rates of reported unfair/poor treatment (often upward of 30%), but something like a microaggression is a more nuanced phenomenon with subtler health implications than, say, burning someone’s house down. I think we need to measure both, and understand the implications for both.
One explanation from my study’s findings is that for Black adults, high awareness or the consequences of systemic racism could override the negative health effects of interpersonal discrimination (especially in areas where you spend less time like the doctor’s office compared to something like work or school). Being overtly disenfranchised through less access to insurance, healthy foods, medical services, etc. could also overcome any nuanced consequence of discrimination. When discriminatory treatment is anticipated, some could follow protective coping strategies for managing those experiences and en route still get the care they need. Some White adults who may not carry that same day-to-day awareness of something that looms as large as systemic racism may find not find discrimination normal. Therefore, ageism, classism, or religion-related bias may land as more unexpected when it happens to them. Through my analysis, it is unclear whether the reported discrimination is directly harmful (e.g. causation). My view is that reported mistreatment can signal poor quality care, even in the event that someone receives excellent care for their physical issues. If the culture of a healthcare setting is not emotionally or culturally welcoming, that experience can still drive a patient away.
In the future I would love to have more data available with more participants. If I can access more representation in my data and also ensure the questions capture consistent responses across populations, I can dig deeper into the consequences of discrimination in healthcare. My study also warrants more investigation into the reasons discrimination is reported. In my data, there are variables which allow participants to describe why they think the discrimination happens to them. However, those attribution variables only apply to the larger Everyday Discrimination Scale, which captures discrimination across many settings outside of healthcare. For example, let’s say someone says police or restaurants treat them poorly because of their race, but hospitals treat them poorly because of their weight. You cannot disentangle these attributions. For my future work, I think it is important to understand not only the source of the discrimination, but also the attributed reason, so that we can understand how it affects health behavior. This shows why discrimination in healthcare is an important issue for all people, especially in our American system where so many people are dissatisfied with their care.